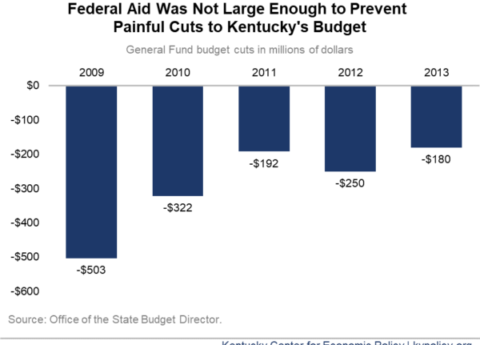
New Survey Shows Extreme Hardship Among Kentuckians as President Halts Talks on New COVID-19 Aid Bill
Yesterday President Trump tweeted that he was ending Congressional talks on a critical new aid package. A new survey of...
Research That Works for Kentucky
Copyright © 2024 KyPolicy Privacy Policy Terms & Conditions Sitemap