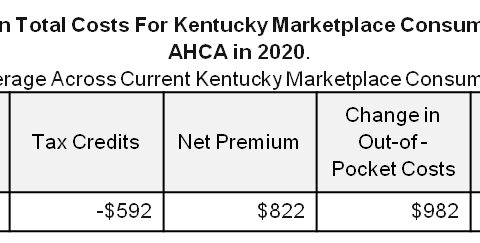
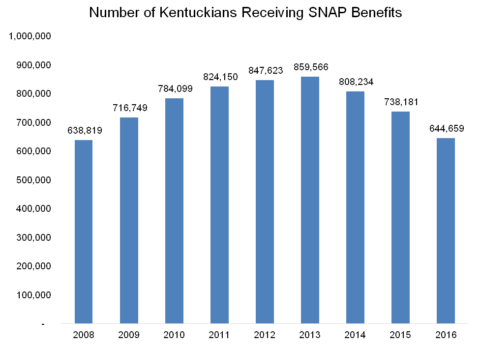
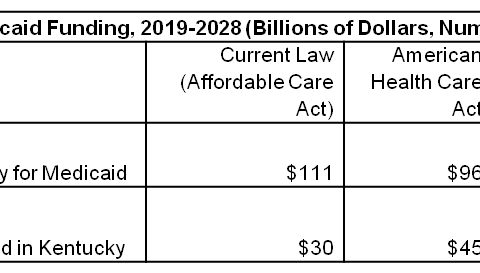
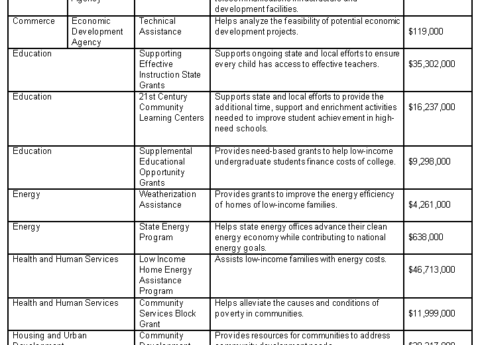
Getting Rid of Essential Health Benefits Means Less Coverage, More Costs for Kentuckians
The House has amended their healthcare repeal to include eliminating a requirement that insurance plans in the individual and small...
Research That Works for Kentucky
Copyright © 2024 KyPolicy Privacy Policy Terms & Conditions Sitemap